Finding the right doctor is a top priority for patients who are diagnosed with mesothelioma. Prompt and proper treatment is the best chance patients have for improving their prognoses and prolonging life. Many experienced oncologists have never treated mesothelioma before. However, patients can find quality care from mesothelioma specialists at hospitals and cancer centers throughout the United States.
Top Mesothelioma Doctors
The following doctors have dedicated a solid portion of their careers to treating and researching malignant mesothelioma.
Raphael Bueno – Pleural Mesothelioma Surgeon

Dr. Bueno is Chief of Thoracic Surgery and Co-director of the Brigham and Women’s Lung Center in Boston.
In addition to performing surgeries, Bueno focuses his research on finding novel methods to diagnose mesothelioma. He was part of a team that found a gene-ratio technique could help not only verify a mesothelioma diagnosis, but could also differentiate what cell types were predominant in the affected tissues. Survival rates are dramatically affected by cell type, making this finding particularly significant for pleural mesothelioma patients.
Get connected with Dr. Bueno
Hedy Lee Kindler – Medical Oncologist for Pleural and Peritoneal Mesothelioma

Dr. Kindler is a renowned mesothelioma specialist at the University of Chicago Comprehensive Cancer Center. She treats hundreds of patients with pleural mesothelioma, lung cancer and pancreatic cancer every year.
Kindler designs and oversees clinical trials looking for novel agents to treat mesothelioma. That includes the development of chemotherapy drugs and angiogenesis inhibitors for mesothelioma patients. She is also active in research efforts involving peritoneal mesothelioma, the second-most common form of the disease.
Kindler is also a past recipient of the Selikoff Lifetime Achievement Award from the Asbestos Disease Awareness Organization.
Get connected with Dr. Kindler
Robert Taylor Ripley – Pleural Mesothelioma Surgeon
 R. Taylor Ripley, MD is the associate professor of surgery at Baylor College of Medicine and director of the Mesothelioma Treatment Center at Baylor St. Luke’s Medical Center. Dr. Ripley is a nationally recognized, board-certified thoracic surgeon and expert in thoracic surgical oncology specializing in treatment of mesothelioma. In addition to mesothelioma, he practices all facets of general thoracic surgery including infectious lung disease and benign esophageal diseases as well as endobronchial, multidisciplinary management of patients with lung, esophageal, thymic, and other thoracic malignancies, and endoscopic interventions. He also specializes in robotic surgery to provide minimally invasive approaches to thoracic diseases.
R. Taylor Ripley, MD is the associate professor of surgery at Baylor College of Medicine and director of the Mesothelioma Treatment Center at Baylor St. Luke’s Medical Center. Dr. Ripley is a nationally recognized, board-certified thoracic surgeon and expert in thoracic surgical oncology specializing in treatment of mesothelioma. In addition to mesothelioma, he practices all facets of general thoracic surgery including infectious lung disease and benign esophageal diseases as well as endobronchial, multidisciplinary management of patients with lung, esophageal, thymic, and other thoracic malignancies, and endoscopic interventions. He also specializes in robotic surgery to provide minimally invasive approaches to thoracic diseases.
Get connected with Dr. Ripley
Why A Mesothelioma Doctor is Important
Mesothelioma is a complex disease. Early detection makes it possible for patients to receive more aggressive therapies and extend life expectancy.
The initial symptoms of mesothelioma are so subtle that it can be mistaken for less serious illnesses. However, a mesothelioma specialist is trained at recognizing telltale symptoms that may be missed by other doctors. Identifying the early signs of mesothelioma may enable patients to be diagnosed in the earlier ― and more treatable — stages of the disease.
A mesothelioma specialist knows the most effective treatment methods for the different forms of the disease. Specialists also stay current on the latest developments in cancer care, including clinical trials that may be beneficial for their patients.
In addition, doctors who routinely care for mesothelioma patients will be able to customize treatments for each individual and detect when changes need to be made to the treatment plan. Because mesothelioma spreads rapidly, it is important to have a physician who can make swift decisions to stop or delay the progression of the disease.
Mesothelioma specialists do not work alone. Most cancer centers adopt a team approach to mesothelioma treatment, where oncologists work alongside top surgeons and other experts to monitor patient care. A specialist can refer patients to other health care providers who have the knowledge and skills needed to tackle an uncommon cancer like mesothelioma.
However, specialists are not found in every state. Patients may need to travel in order to receive care from a mesothelioma doctor. For many, it’s a worthwhile investment. Mesothelioma experts help patients make complicated treatment decisions and start planning for the future. That can bring peace of mind to patients and families during such an uncertain time.
What a Mesothelioma Doctor Can Do
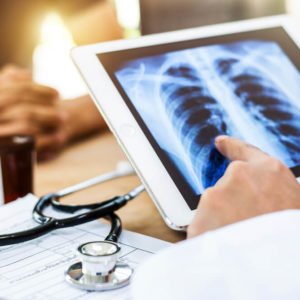
Most mesothelioma patients are referred to oncologists by their family doctor or general practitioner. A family doctor may be able to recognize irregularities in X-rays or other imaging tests, but will most likely not be able to diagnose mesothelioma.
- A mesothelioma doctor can provide comprehensive care for patients. They can:
- Diagnose mesothelioma
- Stage the cancer
- Identify mesothelioma cell type(s)
- Develop a treatment plan
- Coordinate all members of the mesothelioma team
- Seek or provide second opinions
- Inform patients of risks and benefits of treatment(s)
- Explain any possible side effects
- Provide information about clinical trials
- Give opinions about the effectiveness of any alternative therapies that a patient may be considering
Patients should always inform their doctors if they have a history of asbestos exposure. That could guide an oncologist to consider mesothelioma as a possible diagnosis instead of more common cancers.
 Types of Oncologists
Types of Oncologists
There are three main types of oncologists who may be involved in a mesothelioma patient’s care:
- Medical oncologists are usually the first contact person for cancer patients. They specialize in using chemotherapy, targeted therapy, hormonal therapy, immunotherapy and biological therapy to treat cancer. A medical oncologist is usually the doctor who coordinates care for a patient’s mesothelioma team.
- Surgical oncologists perform biopsies and surgeries to help diagnose and treat patients with mesothelioma. A surgical oncologist can also perform palliative care procedures to reduce pain and improve quality of life for patients in the late stages of mesothelioma.
- Radiation oncologists use high-energy radiation to shrink tumors and kill cancer cells.
- A mesothelioma patient may be treated by all three types of oncologists at the same time. This type of treatment is called multimodal therapy.
Mesothelioma doctors tailor the types of treatments that patients receive based on the stage of the cancer and the patient’s overall health. Patients in the late stages of mesothelioma generally have fewer treatment options. However, a mesothelioma specialist may be able to direct patients to experimental therapies that could offer a brighter outlook.
How to Choose the Best Mesothelioma Doctor for You
Selecting the best mesothelioma doctor is a personal decision. Patients and family need to find a physician that they trust during such a turbulent time.
Think of the process of choosing a doctor as a job interview. Qualifications to consider should be:
 Experience
Experience
- Has the doctor treated mesothelioma before? If so, what were the outcomes?
- Does the physician specialize in a certain form of mesothelioma?
- How many cases of mesothelioma does the doctor treat per year?
- Where was the doctor trained?
- What is the doctor’s specialty?
- Does the physician work at a cancer center with a mesothelioma program?
- Is the doctor conducting any mesothelioma research or clinical trials?
Treatment Recommendations
- Does the doctor explain the cancer staging process and what that means for a mesothelioma patient’s prognosis?
- What treatment options does the physician suggest?
- Does the doctor identify more than one possible treatment protocol?
- Did the patient learn what to expect as treatment progresses?
- Is the doctor open to second or third opinions?
- Can the doctor direct the patient to clinical trials that may be appropriate?
Personal Considerations
- Was the patient comfortable with the doctor’s bedside manner?
- Were all of the patient’s questions answered fully?
- Did the appointment feel rushed, or was the doctor thorough?
- Would the patient feel comfortable telling the doctor anything?
- Does the patient know anyone who has been treated by the physician before?
- Did the doctor take the patient’s own preferences into account?
Feasibility
- Would the patient have to travel for treatment? If so, is that practical?
- Is the doctor affordable?
- Can health insurance or government assistance help offset the cost of treatment?
It is important to start cancer treatment as soon as possible after a mesothelioma diagnosis. But patients should not rush into choosing an oncologist. Getting treatment from the right mesothelioma team can reassure patients that everyone is working together for the best possible outcome.
Need Help After a Mesothelioma Diagnosis? Download Our Free Guide
It can be difficult to know where to turn after being diagnosed with mesothelioma. The team at Mesothelioma Help has created a free guide to mesothelioma to support you during your cancer battle.
Download our free guide to receive:
- Legal advice from one of the country’s top-rated mesothelioma attorneys
- Medical recommendations from mesothelioma specialists
- News about recent developments in cancer treatment
- Guidance on finding mesothelioma doctors and hospitals near you
- Advice on how to connect with other courageous mesothelioma patients and caregivers
This guide is a comprehensive resource for patients no matter where they are on their cancer journey.
DOWNLOAD YOUR FREE PATIENT’S GUIDE NOW
Free Mesothelioma Patient & Treatment Guide
We’d like to offer you our in-depth guide, “A Patient’s Guide to Mesothelioma,” absolutely free of charge.
It contains a wealth of information and resources to help you better understand the condition, choose (and afford) appropriate treatment, and exercise your legal right to compensation.
Download Now Types of Oncologists
Types of Oncologists Experience
Experience