Researchers Say P/D Surgery Improves Quality of Life for Pleural Mesothelioma Patients
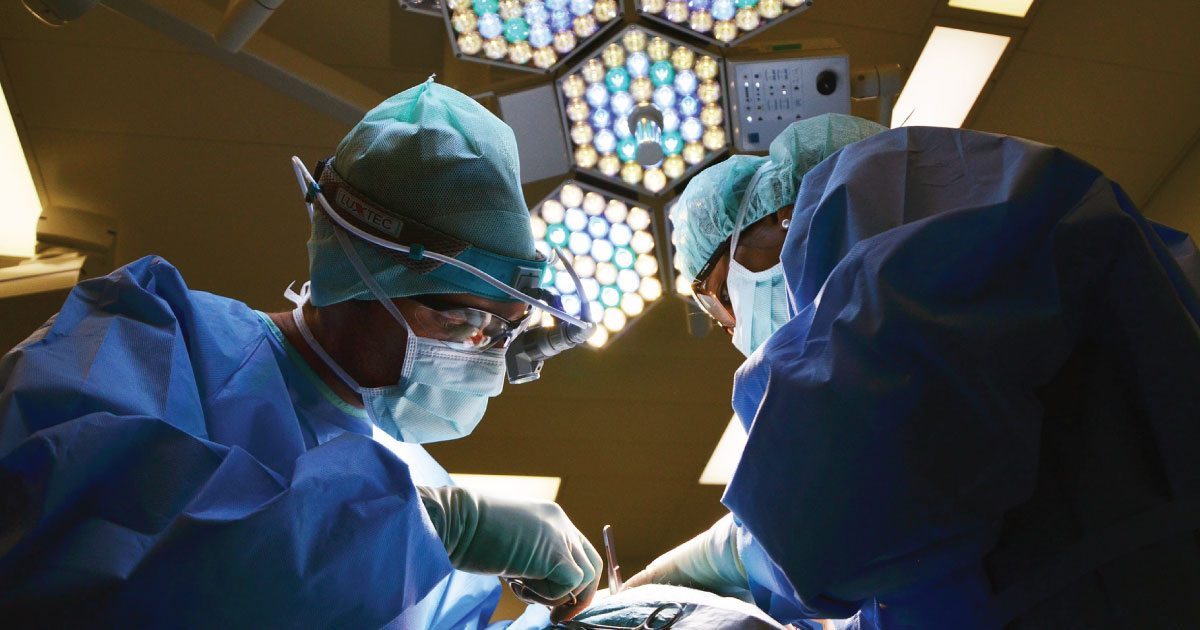
 There are two primary surgical options for pleural mesothelioma patients – pleurectomy/decortication (P/D) or extra pleural pneumonectomy (EPP). Although most mesothelioma experts are solidly in one camp when it comes to favoring a surgery, researchers now report the P/D option can improve physical and emotional quality of life for patients.
There are two primary surgical options for pleural mesothelioma patients – pleurectomy/decortication (P/D) or extra pleural pneumonectomy (EPP). Although most mesothelioma experts are solidly in one camp when it comes to favoring a surgery, researchers now report the P/D option can improve physical and emotional quality of life for patients.
According to a June 9 article by researchers from Loyola University Health System, led by thoracic surgeon, Wickii Vigneswaran, MD, of University Chicago Stritch School of Medicine, mesothelioma patients should not shun P/D surgery for fear it will negatively impact their quality of life. On the contrary, say the researchers, P/D can “help control the buildup of fluid, improve breathing and lessen cancer pain,” thus improving the patient‘s quality of life.
Pleural mesothelioma is a rare, terminal form of cancer affecting the lining of the lungs caused by exposure to airborne asbestos fibers. Although the goal of any mesothelioma surgery is to achieve a macroscopically-complete resection, which refers to the removal of all visible tumor cells, mesothelioma displays as a large mass of interlocked tumors that blend in with healthy tissue, making it difficult to remove the disease in its entirety.
P/D surgery, referred to as lung-sparing surgery, involves removing the diseased membrane lining the lung and stripping away all visible mesothelioma tumors but the lung is not removed. The alternative to P/D is the extra pleural pneumonectomy which is a radical and complex surgery that features the removal of the affected lung and parietal pleura, as well as the possible removal of the diaphragm, the pericardium and other extra pleural tissue.
The researchers conducted a quality of life survey in a group of 114 mesothelioma patients who underwent P/D. Prior to the surgery, 31 percent of the patients were fully functional (0), 65 percent were abble to do light work (1) and four percent of the patients were unable to perform any tasks (2).
The patients responded to the same questionairre at one month, 4-5 months, 7-8 months and 10-11 months. Improved quality of life was observed in the first month after surgery and was maintained at late follow-up in all patients. Quality of life was not adversely affected by surgery at any time in patients mesothelioma treatment who, prior to surgery, had performance status of 1 or 2.
P/D Surgery Involves a Challenging Recovery
Two of our “Faces of Mesothelioma” mesothelioma warriors were initially treated by undergoing pleurectomy/decortication surgery. David Stetler, whose life with mesothelioma was documented by his daughter Amanda Stetler, underwent a nearly 15 hour surgery by surgeons at Penn Medicine. Stetler remained in the hospital recovering from the challenging surgery for nearly two months.
After recovery, however, he went on to celebrate his 60th birthday, enjoy time at the beach with his family and get back to working around the yard before his health took a downturn. Stetler passed away two years after his surgery.
Don Smitley, whose daughter Jennifer Gelsick continues to blog about life before and after mesothelioma, had the P/D surgery at NYU Langone Medical Center in New York City. Smitley, who spent several weeks recovering, said after the surgery he experienced “serious pain,” something he thought he’d never have to endure. He too was able to live nearly 20 more months enjoying life with his family and doing the things he loved, like playing guitar in his bluegrass band and tinkering around the yard.
Dr. Vigneswaran cautions that while the surgery is not a cure, he concluded from the study, “The net benefit of pleurectomy and decortication justifies the procedure in the majority of patients with malignant pleural mesothelioma.”
If you have been diagnosed with pleural mesothelioma, talk to your doctor to determine whether pleurectomy/decortication surgery is right for you.
